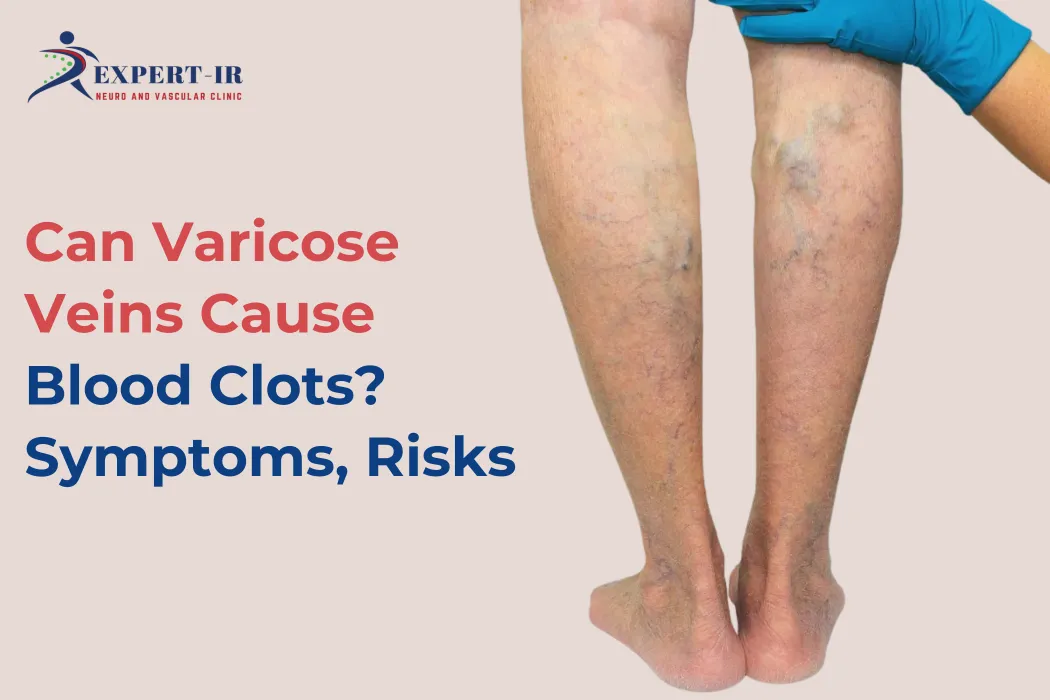
Can Varicose Veins Cause Blood Clots? Symptoms, Risks
Varicose veins are often dismissed as a cosmetic concern, but medically they represent chronic venous insufficiency, it is a condition where blood flow in the veins is impaired. This naturally raises an important clinical question:
Do varicose veins increase the risk of blood clots?
The answer is YES—but not all clots are equally dangerous, and understanding the difference is critical for both patients and early intervention.
Why Clots Form in Varicose Veins?
Blood clots typically form when three conditions occur (known as Virchow’s triad):
- Sluggish blood flow
- Vessel wall damage
- Increased clotting tendency
Varicose veins fulfill two major components of this triad.
Because vein valves fail, blood does not flow efficiently upward. Instead, it pools and stagnates, especially in the lower legs. This slow-moving blood increases the likelihood of clot formation.
At the same time, stretched vein walls become inflamed and damaged, creating an environment that further promotes clotting.
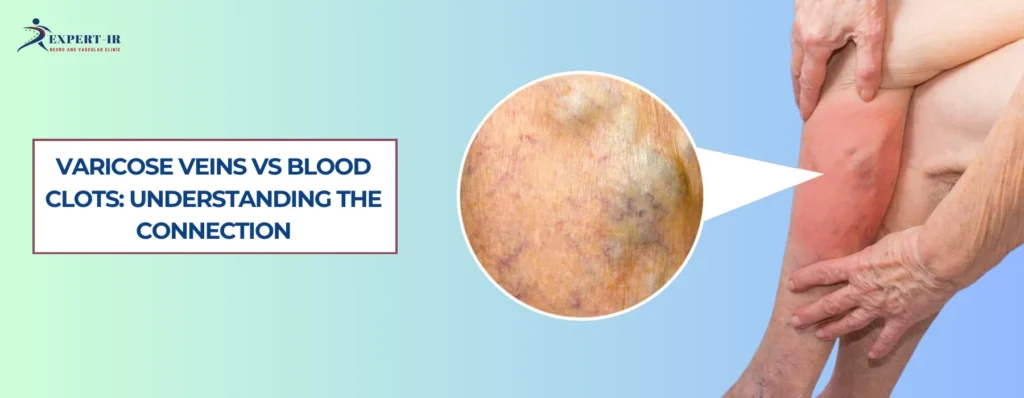
What Type of Clots Are Common in Varicose Veins?
1. Superficial Thrombophlebitis (Most Common)
This is the most frequent clot associated with varicose veins.
It occurs in veins close to the skin and presents with:
- Localized pain
- Redness
- Warmth
- A hard, cord-like vein
While usually not life-threatening, it should never be ignored, as it can extend into deeper veins in some cases.
2. Deep Vein Thrombosis (DVT) – Less Common but Serious
Varicose veins are not the primary cause of DVT, but they can increase the risk slightly, especially when combined with other factors like:
- Prolonged immobility
- Surgery
- Obesity
- Smoking
- Pregnancy
DVT is dangerous because the clot can travel to the lungs, causing a pulmonary embolism.
Warning Signs You Should NOT Ignore
- Sudden swelling in one leg
- Localized redness or warmth
- Sharp or persistent calf pain
- A firm, tender vein
- Skin discoloration or tightening
Emergency signs (possible DVT/PE):
- Sudden breathlessness
- Chest pain
- Rapid heartbeat
These require immediate medical attention.
Does Treating Varicose Veins Reduce Clot Risk?
Yes—this is the most important clinical takeaway.
Treating varicose veins:
- Improves blood flow
- Eliminates pooling
- Reduces inflammation
- Lowers long-term clot risk
Modern treatment focuses on removing the cause, not just symptoms.
Best Treatment to Prevent Clot-Related Complications
Minimally Invasive Treatment
Instead of surgery, current best treatment includes:
Laser Treatment (EVLA)
Seals the faulty vein internally, eliminating blood pooling.
Radiofrequency Ablation (RFA)
Uses controlled heat to close the diseased vein.
These treatments:
- Are performed under local anesthesia
- Allow walking within hours
- Have high long-term success rates
- Significantly reduce complication risks
At Expert IR Neuro & Vascular Clinic, treatment is planned using Doppler-based vein mapping. Dr. Santosh Patil focuses on non-surgical, precision-based vein care that directly reduces clot risk.
Who Is at Highest Risk of Clots with Varicose Veins?
Risk increases significantly when varicose veins are combined with:
- Long sitting (travel, desk job)
- Diabetes
- Obesity
- Smoking
- Hormonal therapy
- Pregnancy
This is where most patients go wrong—they ignore combined risk.
Frequently Asked Questions (FAQs)
Varicose veins increase the risk of superficial blood clots due to slow blood flow and vein inflammation, but they are not the main cause of deep vein thrombosis.
Most clots are superficial and not life-threatening, but they can cause pain and may extend into deeper veins if untreated.
Superficial clots occur in surface veins and are less dangerous, while DVT occurs in deeper veins and can lead to serious complications like pulmonary embolism.
Signs include redness, warmth, swelling, pain, and a hard vein. Sudden swelling or breathing difficulty requires urgent medical care.
Yes. Treating varicose veins improves blood flow and reduces pooling, significantly lowering the risk of clot formation.
For More Details Visit Our Channel
Recent Articles
Is Laser Treatment Safe for Elderly Patients? Risks & Benefits
Can Varicose Veins Cause Blood Clots? Symptoms, Risks
Why Do Varicose Veins Feel Worse in Summer? Causes & Treatment
Is varicose veins surgery risky for diabetic patients?
Ovarian vein reflux occurs when vein valves weaken or fail, allowing blood to flow backward and pool in the pelvic veins. Hormonal changes (especially high estrogen levels), pregnancy, and multiple childbirths increase the risk.
Persistent pain, skin discoloration, non-healing ulcers, and recurrent bleeding are signs of advanced disease requiring urgent evaluation.
Yes. Laser treatment is less invasive, has quicker recovery, and offers high long-term success rates compared to traditional surgery.
A Doppler ultrasound examination determines severity and helps decide whether surgery or minimally invasive treatment is required.
Yes. Advanced cases may lead to ulcers, infections, or blood clots if left untreated.