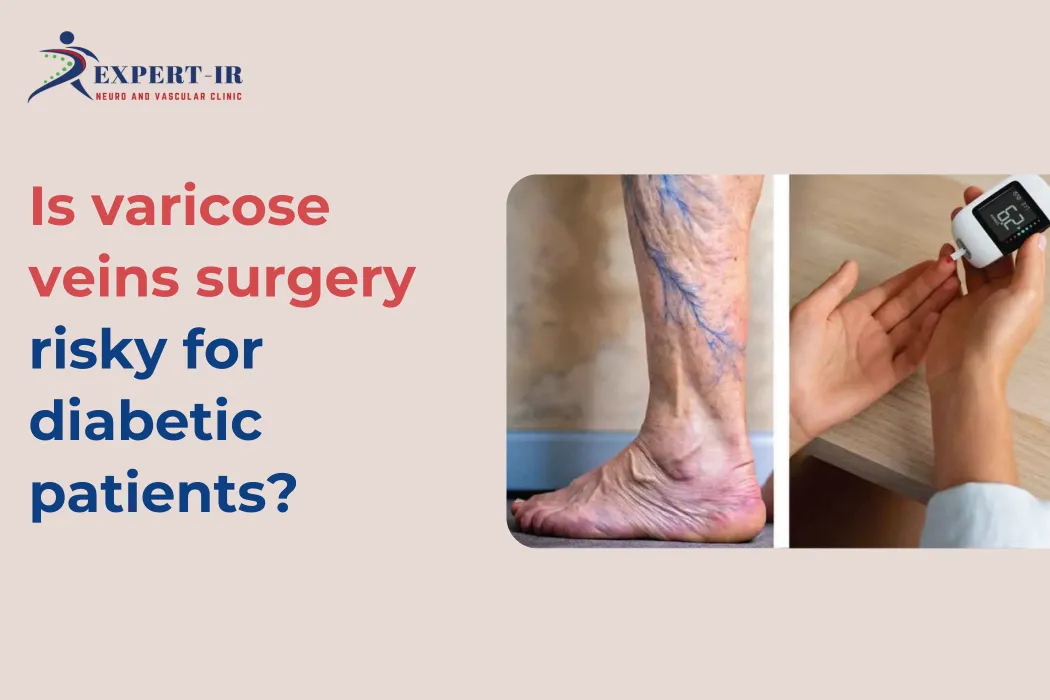
Is varicose veins surgery risky for diabetic patients?
Varicose veins are a common vascular condition, but when a patient also has diabetes, treatment decisions require extra care. One of the most important concerns patients have is: Is varicose veins surgery risky for diabetic patients?
The answer is YES—traditional surgery carries higher risks in diabetic individuals, mainly due to poor wound healing, increased infection risk, and underlying circulation issues. However, the good news is that modern, non-surgical treatments have significantly reduced these risks.
This blog explains why surgery can be risky for diabetic patients, what complications to watch for, and what safer treatment options are available today.
Why Diabetes Increases Surgical Risk
Diabetes affects multiple systems in the body, particularly blood vessels and healing capacity. High blood sugar levels can damage small blood vessels, reducing blood flow to tissues.
This leads to:
- Slower wound healing
- Increased risk of infection
- Reduced immunity
- Higher chances of skin complications
When surgery involves incisions in the legs—where circulation is already compromised—these risks become even more significant.
Varicose Veins Surgery for Diabetic Risks, Recovery & Tips
Delayed Wound Healing
Surgical cuts take longer to heal in diabetic patients due to reduced blood supply. This can prolong recovery and increase discomfort.
Higher Risk of Infection
Diabetes weakens the immune response, making post-surgical infections more likely. Even minor infections can become serious if not treated promptly.
Increased Risk of Skin Breakdown
Fragile skin and poor circulation may lead to complications such as wound opening or tissue damage after surgery.
Risk of Blood Clots
Some diabetic patients have an increased risk of clot formation, which may complicate recovery after surgery.
Non-Surgical Varicose Vein Treatment fpor Diabtic Patients
Endovenous Laser Treatment (EVLA)
Laser treatment seals the faulty vein from inside using heat energy. It does not require large incisions, which significantly reduces infection and healing risks.
Radiofrequency Ablation (RFA)
RFA is another minimally invasive option that uses thermal energy to close the affected vein safely and effectively.
Why Non-Surgical Treatments Are Better for Diabetic Patients
- No large surgical cuts
- Minimal risk of infection
- Faster healing
- Same-day walking
- Reduced complication rate
These advantages make minimally invasive procedures the preferred treatment choice for diabetic patients.
Importance of Expert Evaluation
Before deciding on treatment, a detailed Doppler ultrasound is essential to assess vein function and blood flow.
At Expert IR Clinic, advanced imaging is used to plan safe, personalized treatment. Dr. Santosh Patil specializes in non-surgical vein procedures designed specifically for high-risk patients, including those with diabetes.
Frequently Asked Questions (FAQs)
Yes, diabetic patients can receive varicose vein treatment — and in most cases, they should not delay it. The key is choosing the right approach. Minimally invasive procedures like EVLT and RFA are significantly safer than open surgery for diabetics because they involve no large incisions, no general anaesthesia, and minimal healing requirements.
Traditional surgical stripping requires multiple incisions that must heal properly. In diabetic patients, elevated blood sugar impairs immune function and circulation, causing wounds to heal slowly and increasing the risk of infection, ulcers, and post-operative complications. General anaesthesia also carries higher risk for poorly controlled diabetics due to cardiovascular involvement.
Minimally invasive options particularly EVLT (Endovenous Laser Therapy) and Radiofrequency Ablation (RFA) — are the safest choices for diabetic patients. These are performed through a tiny needle puncture under local anaesthesia, with no incisions, no hospital stay, and very low risk of infection or healing complications. At Expert IR Clinic Pune, these are the primary treatments used for diabetic patients.
Yes. Diabetes damages blood vessel walls and reduces circulation efficiency, which accelerates the progression of venous insufficiency — the root cause of varicose veins. Diabetic patients often develop symptoms and complications like skin changes and ulcers faster than non-diabetic patients with the same degree of vein disease.
Most interventional radiologists require an HbA1c below 8% and a fasting blood sugar below 180 mg/dL on the day of the procedure before proceeding with elective treatment. Well-controlled diabetes greatly reduces procedural risk and improves post-treatment healing. Individual assessment is always done to determine readiness.
For More Details Visit Our Channel
Recent Articles
Why Do Varicose Veins Feel Worse in Summer? Causes & Treatment
Is varicose veins surgery risky for diabetic patients?
Heavy Menstrual Bleeding & Fibroids | Causes & Treatment
Are Varicose Veins More Common After Pregnancy? Causes
Ovarian vein reflux occurs when vein valves weaken or fail, allowing blood to flow backward and pool in the pelvic veins. Hormonal changes (especially high estrogen levels), pregnancy, and multiple childbirths increase the risk.
Persistent pain, skin discoloration, non-healing ulcers, and recurrent bleeding are signs of advanced disease requiring urgent evaluation.
Yes. Laser treatment is less invasive, has quicker recovery, and offers high long-term success rates compared to traditional surgery.
A Doppler ultrasound examination determines severity and helps decide whether surgery or minimally invasive treatment is required.
Yes. Advanced cases may lead to ulcers, infections, or blood clots if left untreated.