Why Does Leg Swelling Increase During Travel? Causes & Prevention
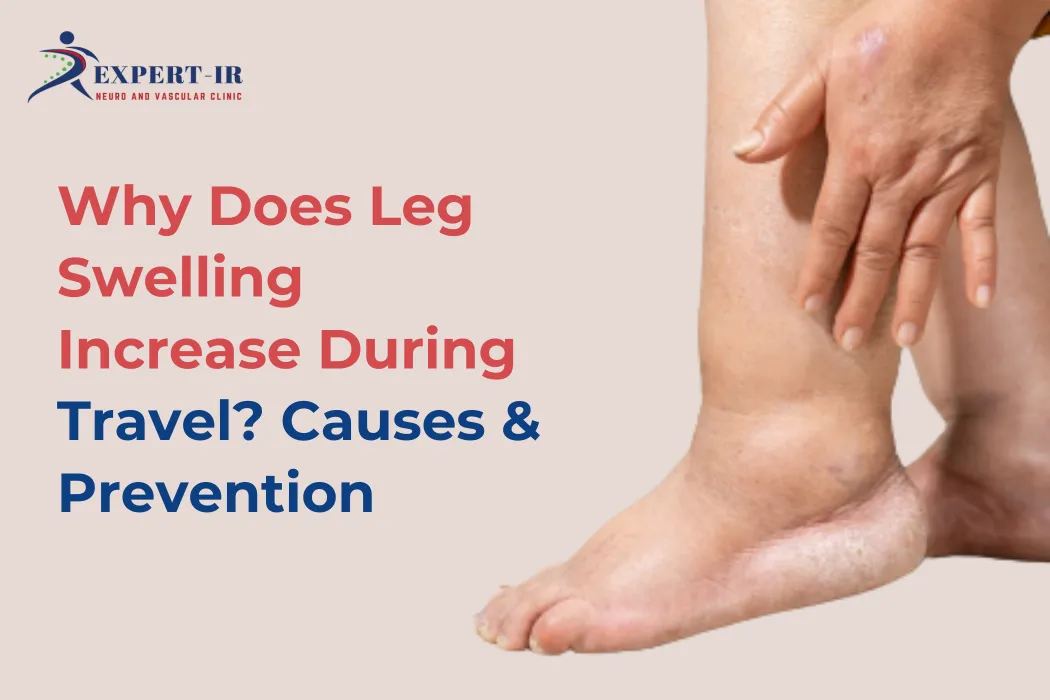
Traveling, whether for work or leisure, often involves long hours of sitting in flights, trains, or cars. While the journey may be exciting, many people notice an uncomfortable side effect—swelling in the legs and feet. This condition, commonly experienced during or after long trips, can range from mild discomfort to a sign of an underlying vascular issue.
Understanding why leg swelling increases during travel is essential not only for comfort but also for preventing potential health complications. With the right awareness and precautions, this issue can be effectively managed and even avoided.
What Happens to Your Legs During Travel?
When you remain seated for extended periods, your body’s natural blood circulation slows down. The calf muscles, which act as a pump to push blood back toward the heart, become inactive. As a result, blood and fluids tend to accumulate in the lower limbs.
Gravity further worsens the situation. Since your legs are in a downward position for hours, fluid retention increases in the feet and ankles. This leads to visible swelling, tightness, and sometimes even a heavy sensation in the legs.
In most cases, this swelling is temporary and resolves once you start moving again. However, repeated episodes should not be ignored.

Causes of Leg Swelling During Travel
- One of the biggest reasons for leg swelling is prolonged immobility. Sitting in a confined space without stretching or walking restricts blood flow, causing fluid to pool in the legs.
- Another contributing factor is dehydration. During travel, people often drink less water and consume more caffeine or alcohol. This imbalance can lead to fluid retention, making swelling more noticeable.
- Air travel adds another layer of complexity. Reduced cabin pressure and lower oxygen levels can slightly affect circulation especially during long-haul flights.
- Individuals with existing vein conditions such as Varicose Veins may experience more pronounced swelling because their veins are already weakened. Similarly, those at risk of Deep Vein Thrombosis should be particularly cautious, as prolonged sitting can increase the chances of clot formation.
Who Is at Higher Risk?
- Existing venous disease — Varicose veins or chronic venous insufficiency means your venous valves are already compromised. Even a short flight can cause noticeable leg swelling or discomfort.
- Previous DVT or pulmonary embolism — If you’ve had a clot before, your risk of another during travel is substantially higher. You need a management plan before any long trip.
- Pregnancy — Increased blood volume, pressure on pelvic veins, and hormonal changes all increase swelling and clot risk.
- Obesity — Higher venous pressure at baseline, compounded by the mechanical compression of travel seating.
- Older age — Venous wall tone and valve competence decrease with age, making pooling more likely.
- Recent surgery or injury — Especially procedures involving the lower limbs, pelvis, or abdomen. The combination of post-surgical clot risk and travel immobility is dangerous.
When Does Swelling Become Dangerous?
Mild, symmetric swelling in both ankles after a long journey is usually benign. It typically resolves within hours of walking around and elevating your legs.
These signs are different:
- Swelling in only one leg — this asymmetry is the classic early warning of DVT
- Calf pain or tenderness, especially when you flex your foot
- Skin that’s warm, red, or discolored on one leg
- Swelling that doesn’t go down after 24–48 hours of rest and normal activity
- Shortness of breath, chest pain, or rapid heartbeat — these can indicate a pulmonary embolism, which is a medical emergency
DVT doesn’t always announce itself dramatically. Some patients have minimal leg swelling and only discover a clot on an ultrasound. This is why any unilateral leg swelling after long-distance travel deserves medical evaluation — not a “wait and see” approach.
How to Prevent Leg Swelling During Travel
- Preventing leg swelling starts with maintaining proper blood circulation throughout your journey. Regular movement is key. Even simple actions like stretching your legs, rotating your ankles, or taking short walks can make a significant difference.
- Hydration plays an equally important role. Drinking enough water helps maintain fluid balance and reduces the risk of swelling. Limiting alcohol and caffeine intake can further support healthy circulation.
- Wearing compression stockings is highly effective, especially for long trips. These stockings apply gentle pressure to the legs, helping blood flow more efficiently and preventing fluid buildup.
- Choosing comfortable clothing can also help. Tight clothes can restrict blood flow, so opting for loose and breathable fabrics is advisable.
- Whenever possible, elevating your legs during breaks can reduce fluid accumulation and improve comfort.
Link Between Travel and Vein Health
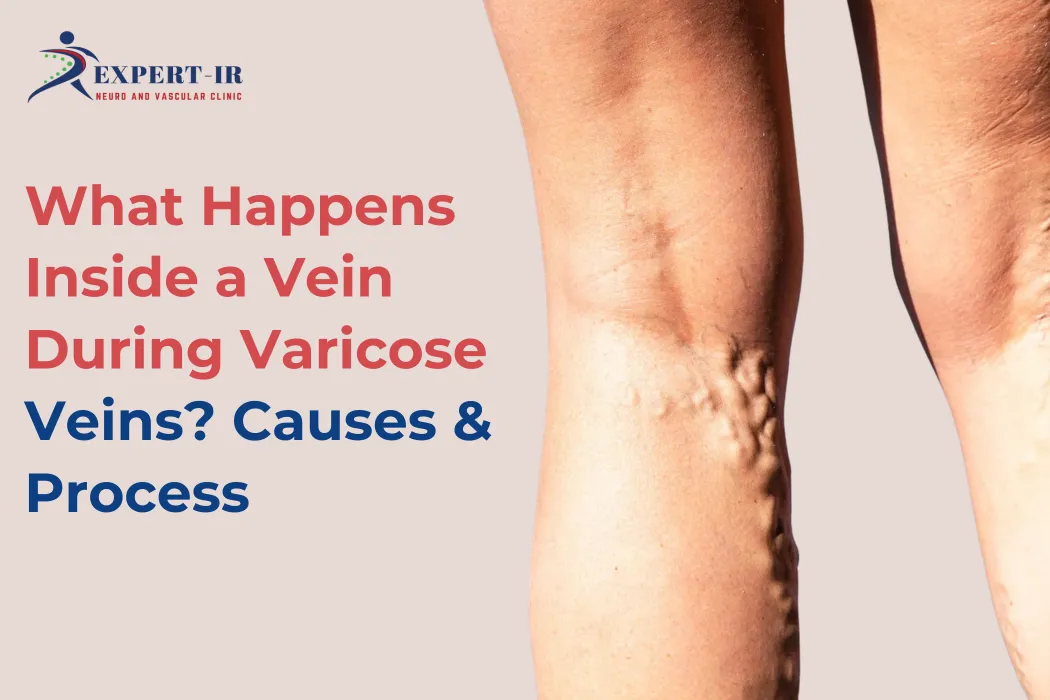
Travel-related leg swelling is often more than just a temporary inconvenience. It can be an early sign of underlying vein problems. Conditions like varicose veins tend to worsen with prolonged sitting and lack of movement.
Ignoring repeated swelling episodes can lead to complications over time. Regular evaluation by a vascular specialist can help detect issues early and prevent further progression.
Maintaining good vein health is especially important for frequent travelers and individuals with pre-existing conditions.
Recovery After Travel
In most cases, leg swelling reduces within a few hours after resuming normal activity. Walking, gentle exercise, and elevating the legs can help speed up recovery.
For elderly patients or those with underlying health conditions, recovery may take slightly longer. Consistent care, hydration, and movement are essential for restoring normal circulation.
If swelling persists or worsens, medical advice is the best course of action.
Frequently Asked Questions (FAQs)
Legs swell due to prolonged sitting, reduced blood circulation, and fluid accumulation in the lower limbs during travel.
Mild swelling is usually harmless, but symptoms like pain, redness, or one-sided swelling may indicate a serious condition like DVT.
Move regularly, stay hydrated, wear compression stockings, and avoid tight clothing to prevent swelling.
Older adults, pregnant women, overweight individuals, and people with vein conditions are more prone to swelling.
Yes, prolonged sitting can worsen varicose veins and increase swelling due to poor blood circulation.
For More Details Visit Our Channel
Recent Articles
Why Does Leg Swelling Increase During Travel? Causes & Prevention
Is Laser Treatment Safe for Elderly Patients? Risks & Benefits
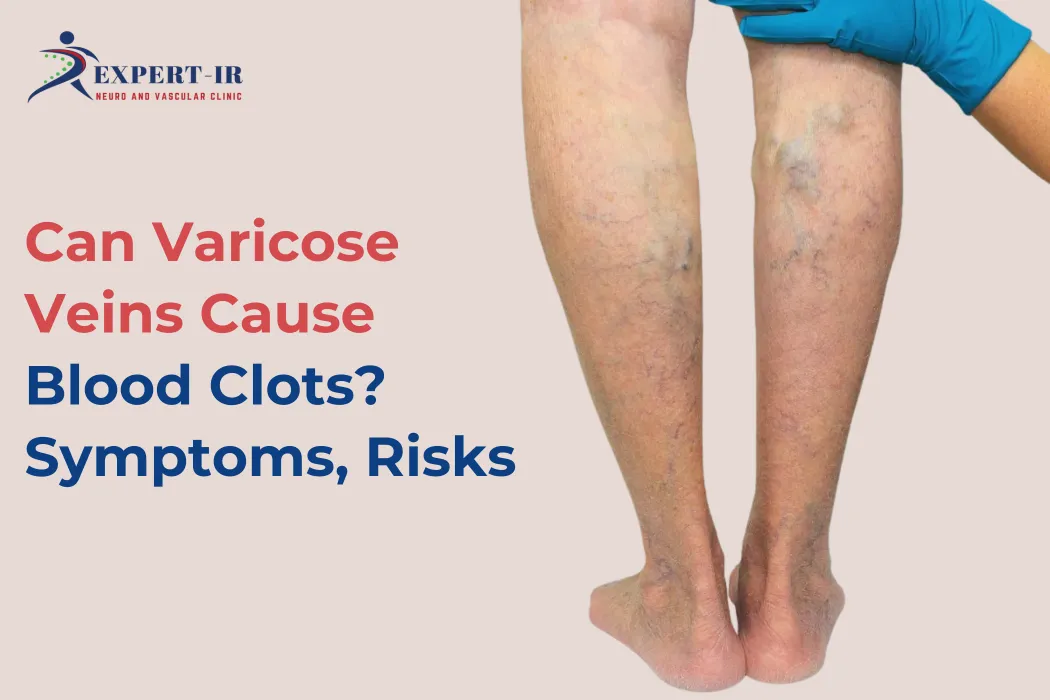
Can Varicose Veins Cause Blood Clots? Symptoms, Risks
Ovarian vein reflux occurs when vein valves weaken or fail, allowing blood to flow backward and pool in the pelvic veins. Hormonal changes (especially high estrogen levels), pregnancy, and multiple childbirths increase the risk.
Persistent pain, skin discoloration, non-healing ulcers, and recurrent bleeding are signs of advanced disease requiring urgent evaluation.
Yes. Laser treatment is less invasive, has quicker recovery, and offers high long-term success rates compared to traditional surgery.
A Doppler ultrasound examination determines severity and helps decide whether surgery or minimally invasive treatment is required.
Yes. Advanced cases may lead to ulcers, infections, or blood clots if left untreated.