Are Varicose Veins More Common After Pregnancy? Causes | Treatment
Pregnancy brings many physical changes to a woman’s body, and one common concern that many new mothers notice is the appearance of varicose veins in the legs. For some women, these veins develop during pregnancy, while others notice them becoming more prominent after delivery. This raises an important question: Are varicose veins more common after pregnancy?
The answer is YES. Pregnancy significantly increases the risk of developing varicose veins due to hormonal changes, increased blood volume, and pressure on the veins of the lower body. Understanding why this happens and how it can be treated helps women protect their vein health after childbirth.
Why Pregnancy Increases the Risk of Varicose Veins?
During pregnancy, the body undergoes major hormonal and circulatory changes to support the growing baby. These changes affect the veins in several ways.
First, blood volume increases to nourish the developing fetus. This additional blood flow puts extra pressure on the veins in the legs. At the same time, pregnancy hormones relax the walls of blood vessels, making vein valves weaker and less efficient.
As the uterus expands, it presses against pelvic veins, slowing the return of blood from the legs to the heart. This leads to blood pooling in leg veins, causing them to enlarge and form varicose veins.

When Do Varicose Veins Appear During Pregnancy?
Varicose veins can appear at any stage of pregnancy, but they are more commonly noticed during the second or third trimester. As the baby grows and weight increases, pressure on the pelvic veins becomes greater.
Some women may also notice spider veins or mild swelling in the early months, which can gradually progress to visible varicose veins later in pregnancy.
Why Varicose Veins Sometimes Appear After Delivery
- While some pregnancy-related varicose veins improve after childbirth, others remain visible or even worsen after delivery. This happens because the veins have already been stretched and the valves weakened during pregnancy.
- Post-pregnancy lifestyle factors such as prolonged standing, weight retention, and reduced physical activity while recovering from childbirth may also contribute to persistent vein problems.
- For women with a genetic tendency toward varicose veins, pregnancy often acts as a trigger that reveals the condition.
- Many women initially notice visible blue or purple veins on the legs. However, symptoms can go beyond cosmetic changes.
- Common symptoms include a feeling of heaviness or fatigue in the legs, swelling around the ankles, throbbing or aching pain, burning sensations, and itching around the affected veins. Symptoms often worsen after long periods of standing or toward the end of the day.
Do Varicose Veins Go Away After Pregnancy?
In mild cases, varicose veins may gradually improve within a few months after childbirth as hormone levels normalize and pressure on the veins decreases.
However, if veins remain enlarged after several months, they may require medical evaluation. Persistent varicose veins indicate ongoing venous insufficiency, which does not resolve without treatment.
How Varicose Veins Are Diagnosed In Pregnancy
Modern diagnosis involves a Doppler ultrasound, which evaluates blood flow in the veins and identifies valve failure. This test helps doctors determine the severity of the condition and select the most appropriate treatment.
Early diagnosis prevents progression and complications such as skin discoloration, eczema, or venous ulcers.
Types of Varicose Treatment During Pregnancy
Today, most varicose veins can be treated without surgery using minimally invasive techniques.
Endovenous Laser Treatment
Laser treatment seals the faulty vein using controlled heat energy. Once closed, blood is redirected through healthy veins, improving circulation and relieving symptoms.
Radiofrequency Ablation
Radiofrequency energy can also be used to close damaged veins. This procedure is safe, effective, and allows quick recovery.
Lifestyle Support
Regular walking, leg elevation, maintaining a healthy weight, and wearing compression stockings may reduce symptoms and support vein health.
At Expert IR Clinic, advanced non-surgical treatments are used to treat varicose veins effectively. Dr. Santosh Patil specializes in minimally invasive vein procedures that help women recover quickly and regain comfort after pregnancy.
Can Varicose Veins Be Prevented After Pregnancy?
While pregnancy-related vein changes cannot always be prevented, certain habits can reduce the risk of worsening symptoms.
Regular physical activity improves circulation, avoiding prolonged standing or sitting reduces venous pressure, and elevating the legs when resting helps blood flow back toward the heart.
Maintaining a healthy body weight after pregnancy also plays an important role in protecting vein health.
Frequently Asked Questions (FAQs)
Yes. Pregnancy significantly increases the risk of varicose veins due to hormonal changes and increased pressure on leg veins.
Some mild cases improve within a few months after delivery, but persistent veins may require medical treatment.
Each pregnancy increases pressure on leg veins, and repeated stretching of veins can weaken valves further.
Yes. Minimally invasive treatments such as laser or radiofrequency ablation are safe and effective once pregnancy and breastfeeding considerations are evaluated.
Varicose veins usually do not affect pregnancy outcomes, but symptoms may worsen during future pregnancies if untreated.
For More Details Visit Our Channel
Recent Articles
Is Laser Treatment Safe for Elderly Patients? Risks & Benefits
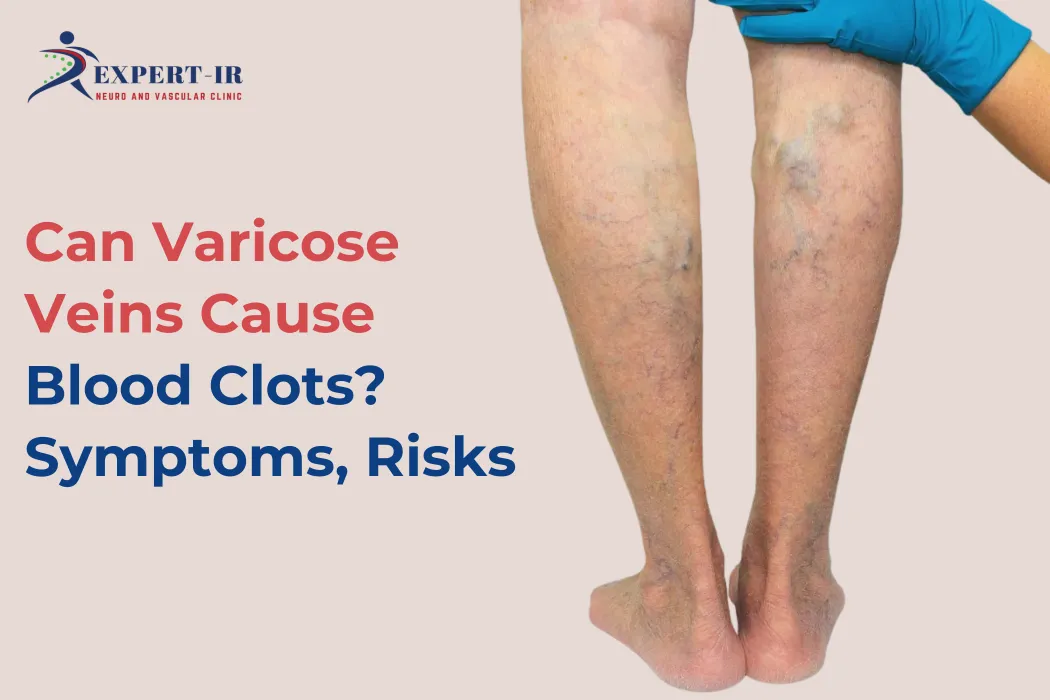
Can Varicose Veins Cause Blood Clots? Symptoms, Risks
Why Do Varicose Veins Feel Worse in Summer? Causes & Treatment
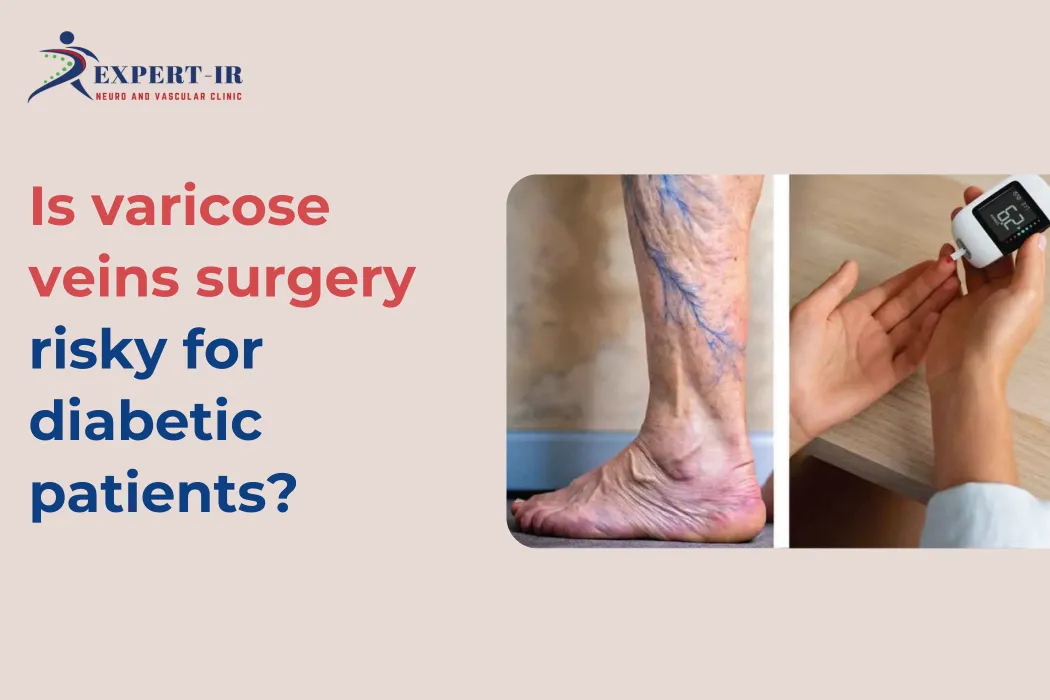
Is varicose veins surgery risky for diabetic patients?
Ovarian vein reflux occurs when vein valves weaken or fail, allowing blood to flow backward and pool in the pelvic veins. Hormonal changes (especially high estrogen levels), pregnancy, and multiple childbirths increase the risk.
Persistent pain, skin discoloration, non-healing ulcers, and recurrent bleeding are signs of advanced disease requiring urgent evaluation.
Yes. Laser treatment is less invasive, has quicker recovery, and offers high long-term success rates compared to traditional surgery.
A Doppler ultrasound examination determines severity and helps decide whether surgery or minimally invasive treatment is required.
Yes. Advanced cases may lead to ulcers, infections, or blood clots if left untreated.